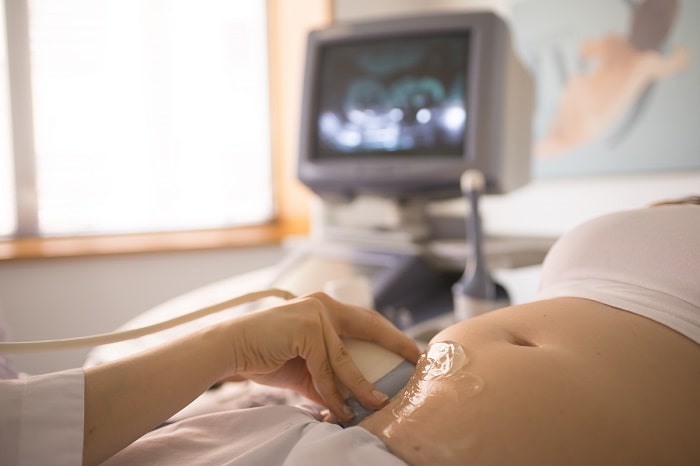
IA EMBRYOSELECT. Embryo Selection with Time-Lapse and Artificial Intelligence
The most advanced embryo culture technology and artificial intelligence come together to select the embryo with the highest reproductive potential, increasing your chances of pregnancy.