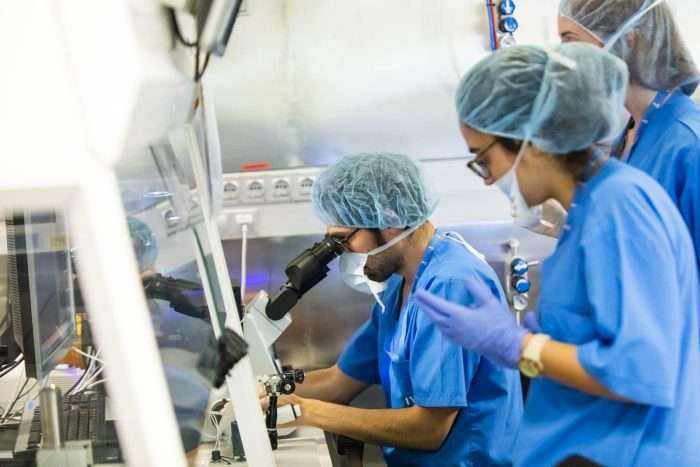
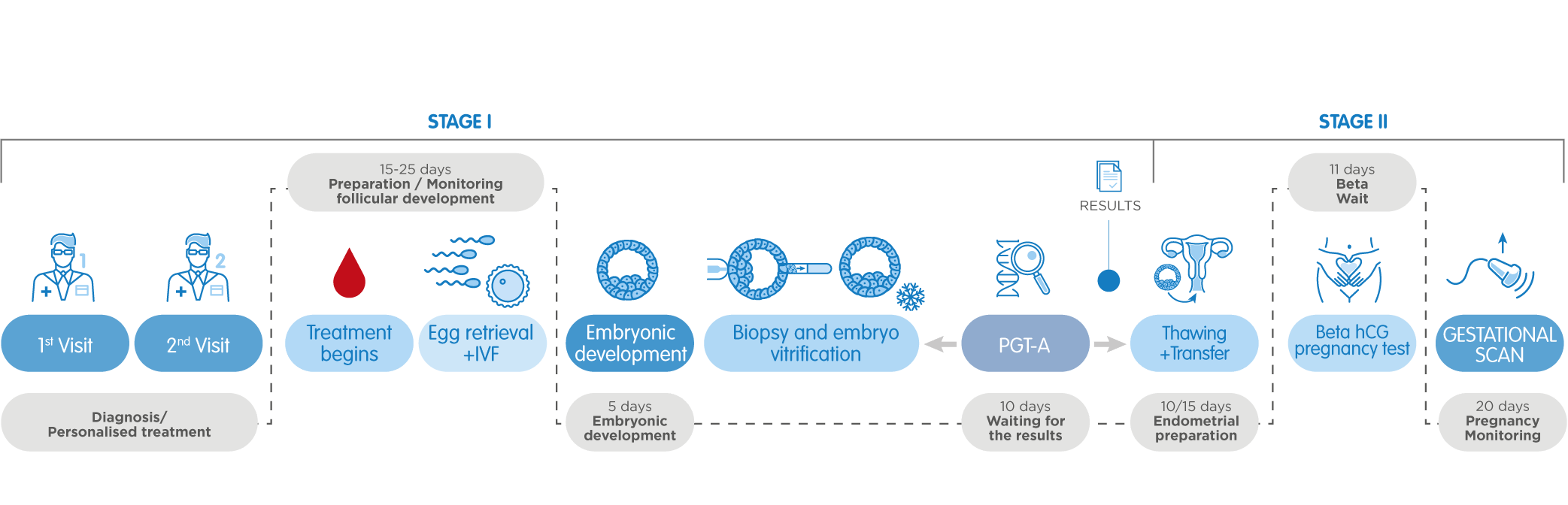
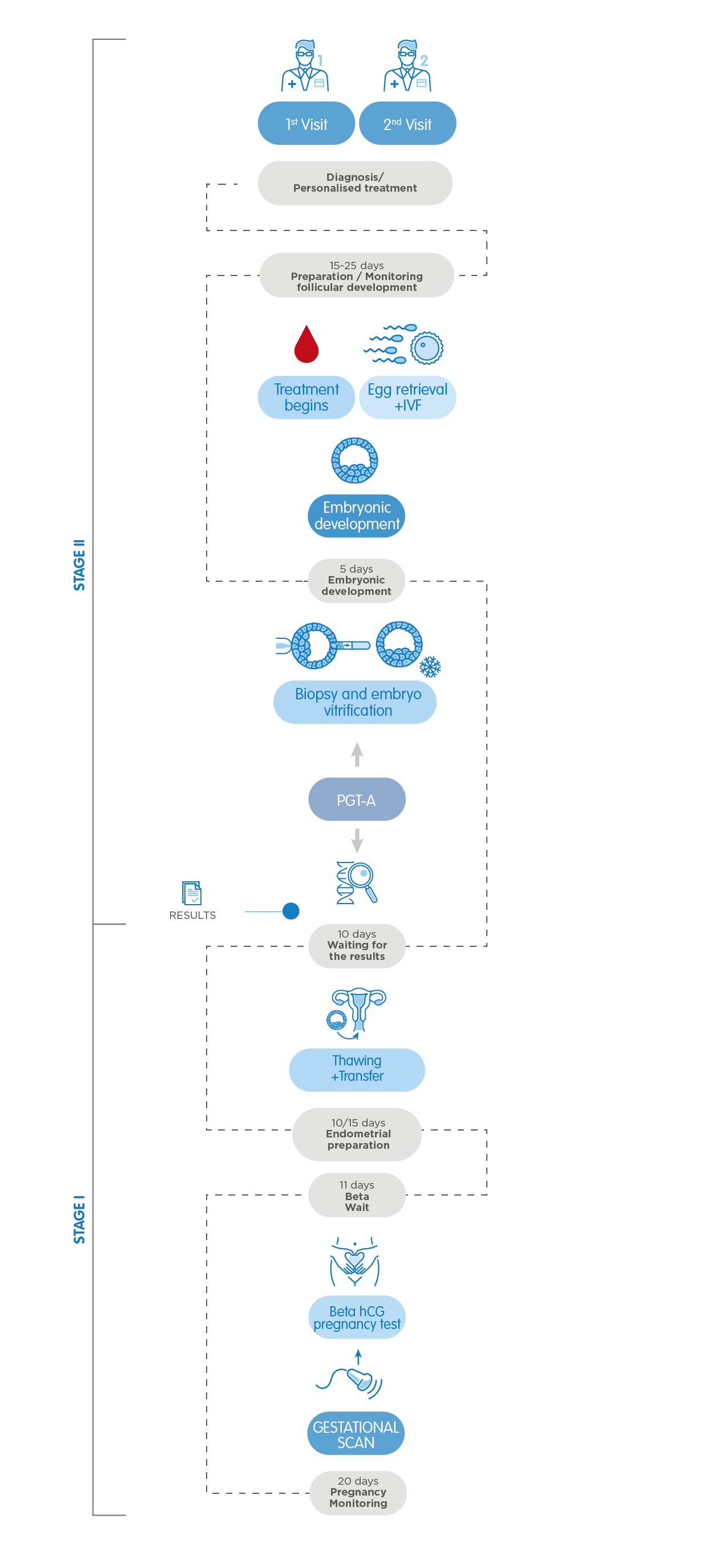
Genetic IVF (IVF + PGT-A)
It is the combination of IVF (In Vitro Fertilization) and PGS (Preimplantation Genetic Screening). Although both techniques have been used for a long time, IVI now offers them in very favourable conditions to ensure, even more so if possible, the safety of its patients' newborn babies.