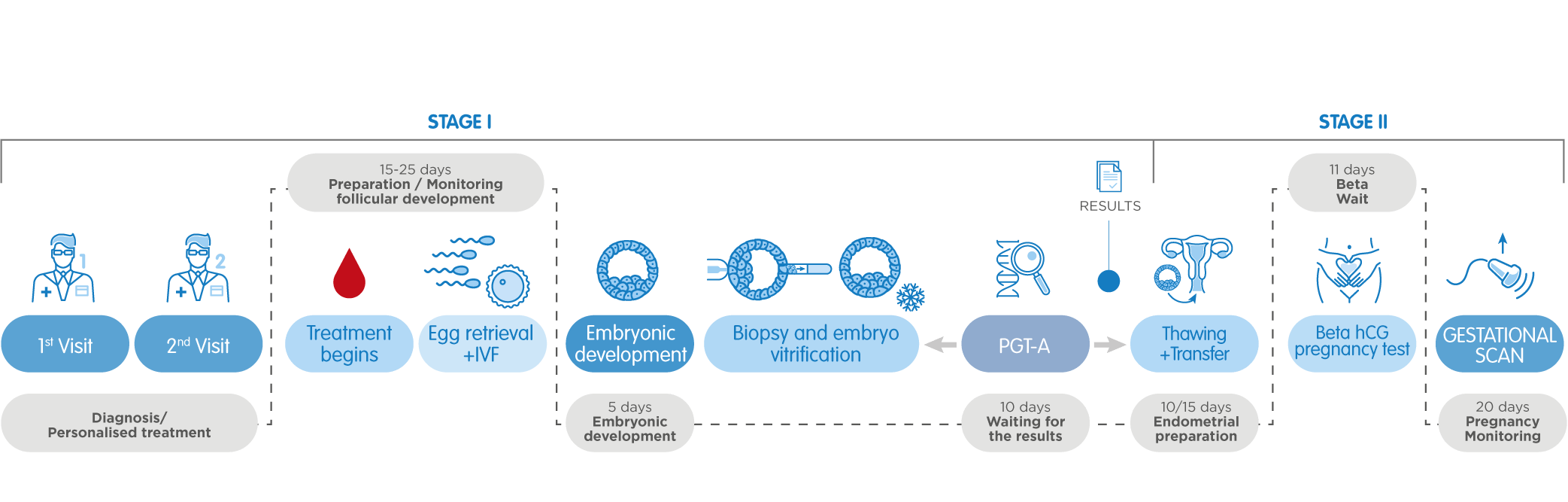
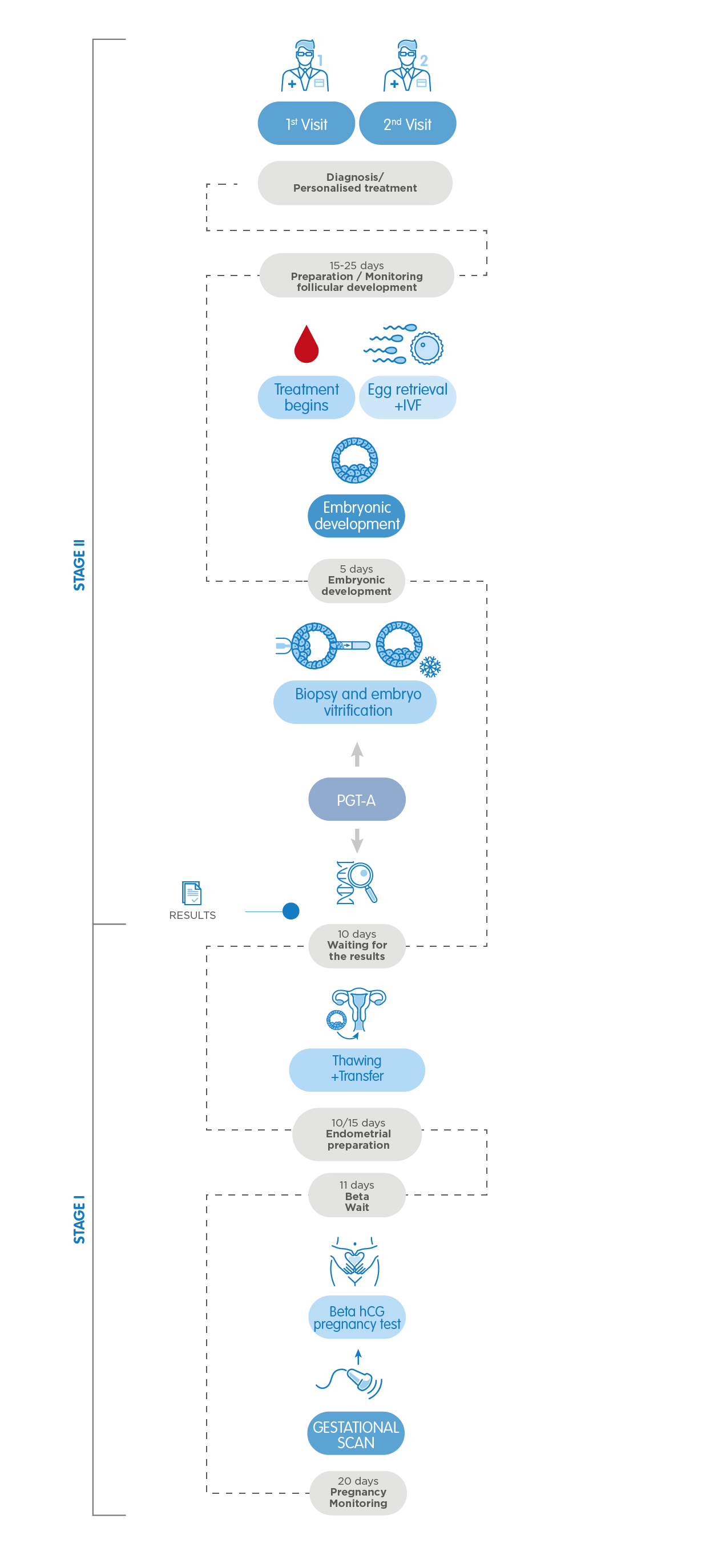
- PGT-A , Preimplantation Genetic Testing for aneuploidy
It helps detect if there are extra or missing chromosomes, a condition known as a numerical abnormality, which is the same as aneuploidy. For example, one suffers from the Down syndrome when instead of having two chromosomes of each, in the chromosome 21 there are three (trisomy 21). Other chromosomal aneuploidies which result in genetic disorders are: trisomy 18, trisomy 13, 45X (Turner syndrome), 47XXY (Klinefelter syndrome), 47XYY y 47XXX.
Recommendations:
- Advanced maternal age: 35 or older.
- Women who suffered two or more miscarriages
- Women after two or more failed in vitro fertilisation cycles.
- Male factor: substantial alterations of sperm parameters may indicate the presence of an altered number of chromosomes in the sperm cells.
- Couples who experienced an altered number of chromosomes during a previous pregnancy.
- Couples who are carriers of numerical abnormalities in the sex chromosomes (X or Y).
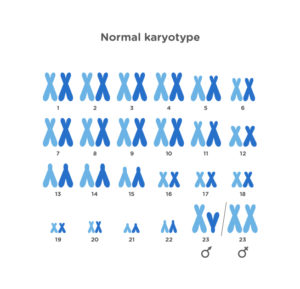
The number of chromosomes of this cell (karyotype) is normal, a total of 46 divided into 23 pairs: 22 autosomes and 1 pair of sex chromosomes. If it is an XX, we are talking about a female, if an XY, about a male.
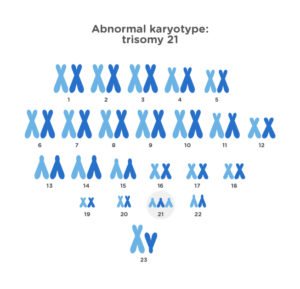
However, the chromosome number of this cell is altered, as instead of 46 chromosomes it has 47, because the pair number 21 contains three copies instead of two, which indicates the Down syndrome.
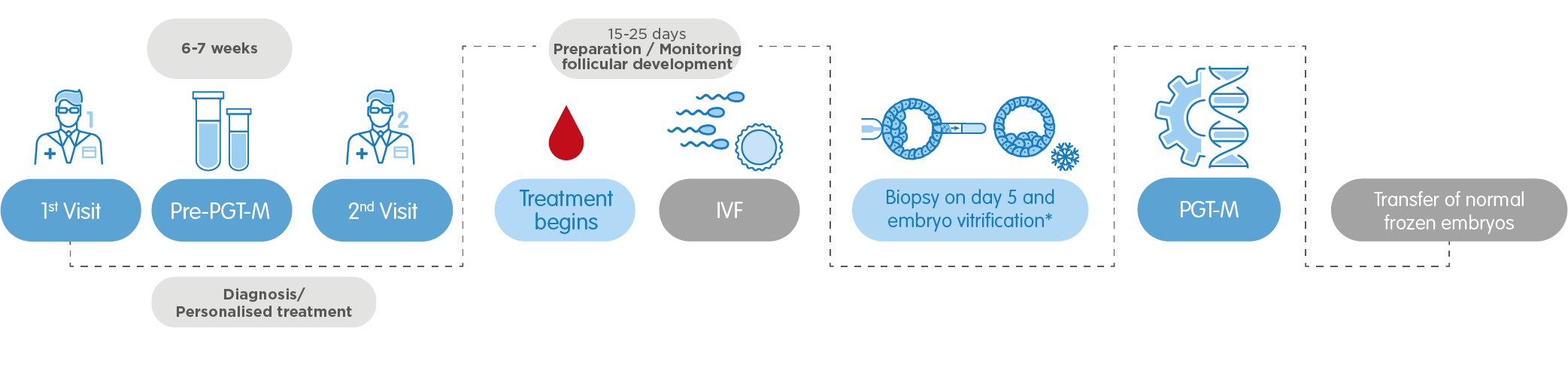
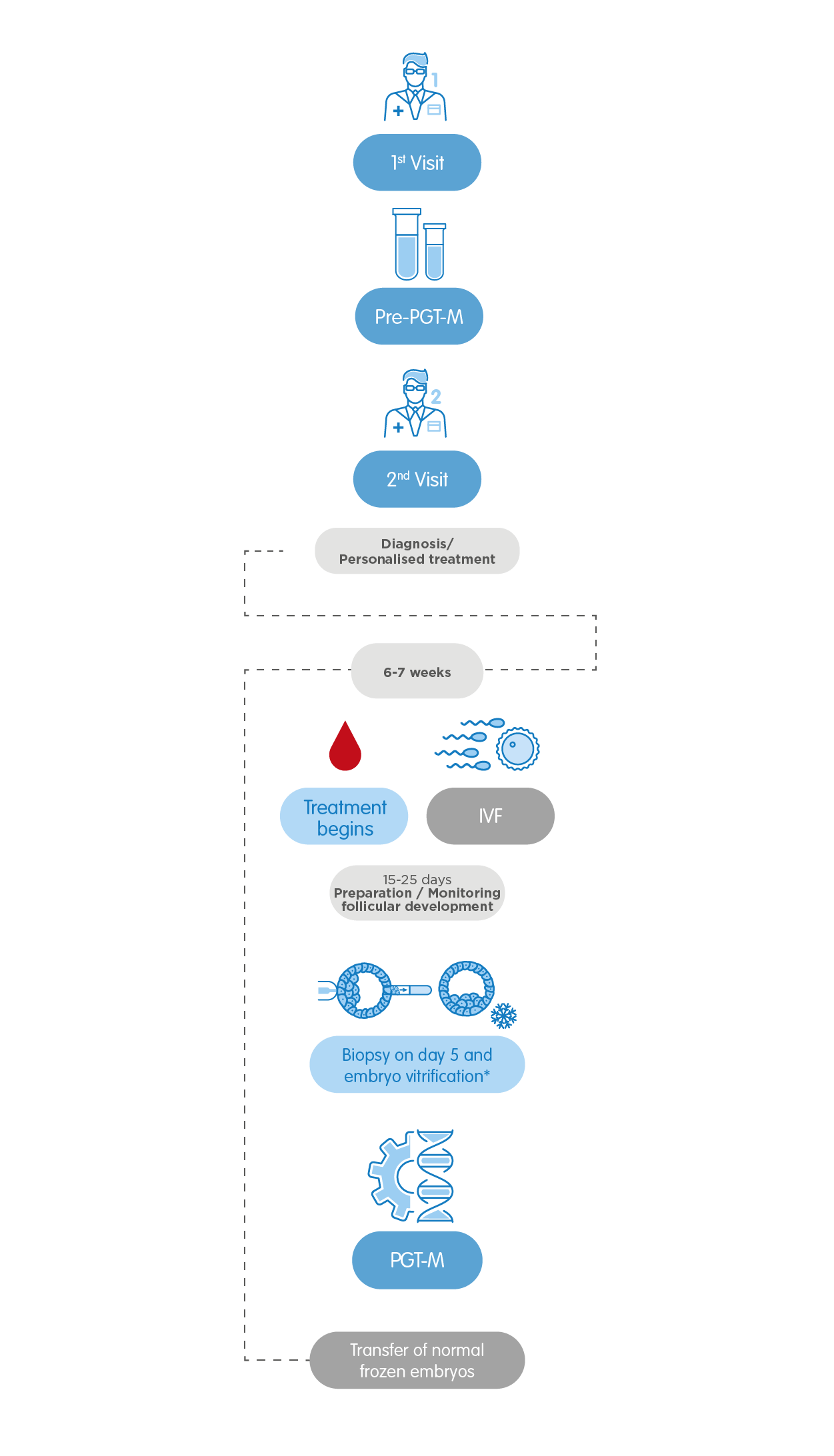
2. PGT-M, Preimplantation Genetic Testing for monogenic (single-gene) disorders
It allows for detecting alterations or mutations of a single gene in the embryos, which may cause a monogenic disorder, also called Mendelian inheritance. The test analyses different types of hereditary diseases: autosomal recessive, autosomal dominant and X-linked disorders, such as cystic fibrosis, Huntington´s disease, Fragile X syndrome, hemophilia A, sickle cell anemia or the Mafran syndrome.
Recommendations:
- One of the members of the couple diagnosed with a genetic disorder.
- Couples in which both members are unaffected carriers of the same genetic condition.
- Family history of a genetic disorder.
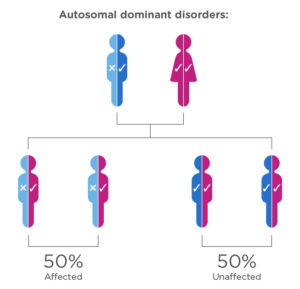
In the case of autosomal dominant disorders, one of the parents carries the affected gene and suffers from the disease (the male in our example). The female´s gene is unaffected. 50% of their offspring will be unaffected and 50% will inherit the mutated gene and therefore suffer from the disease.
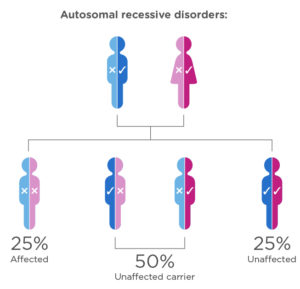
On the contrary, while dealing with autosomal recessive disorders, having just one of the affected copies of the gene does not translate into suffering from the disease, but into being a carrier. To suffer from the condition, both the maternal and the paternal copies must have the mutated gene. In this case, 25% of the offspring will be unaffected, 50% will become unaffected carriers and 25% will be affected by the disease.
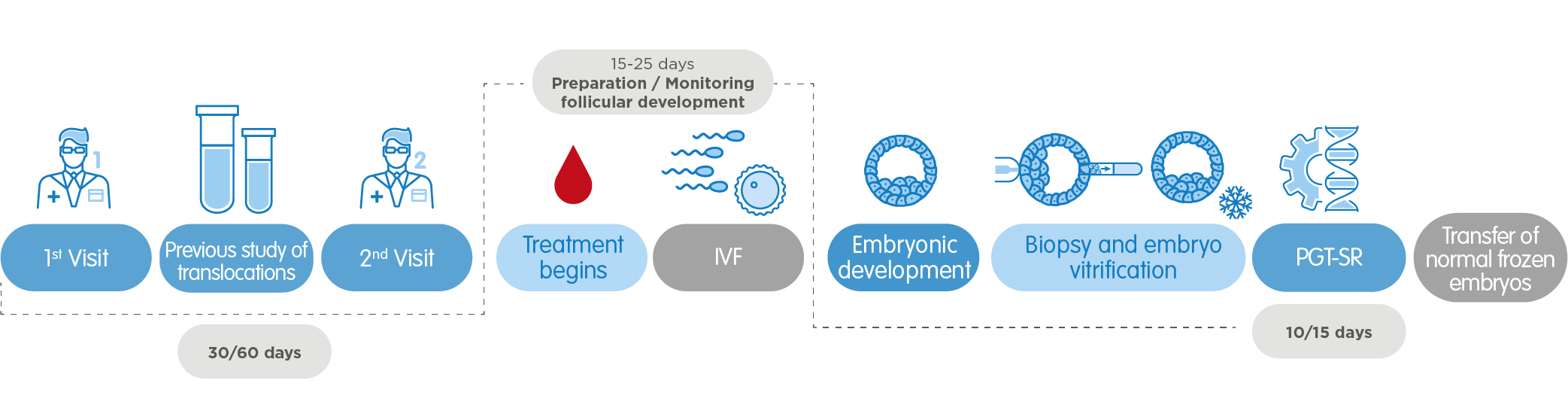
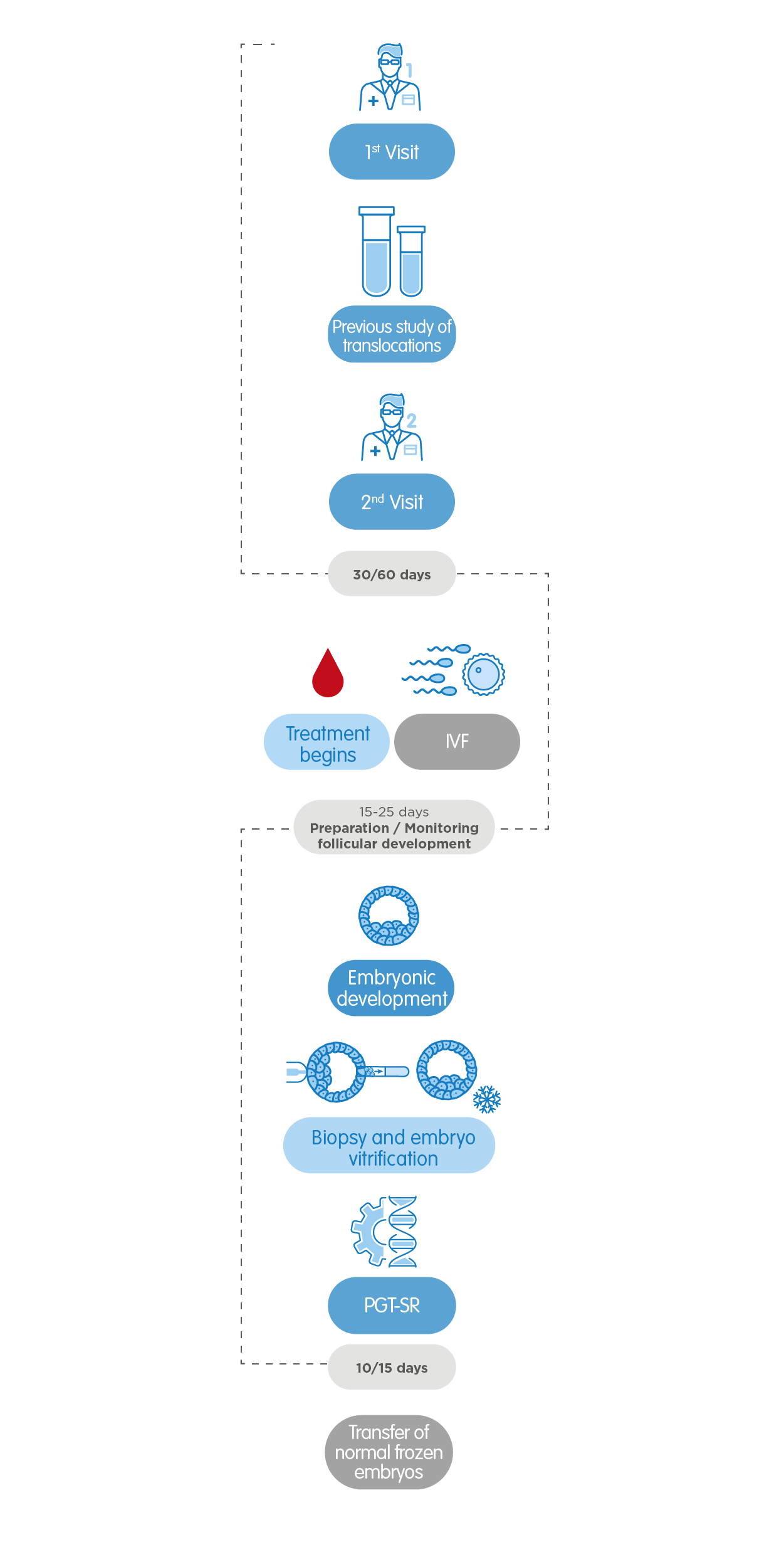
3. PGT-SR, Preimplantation Genetic Testing for structural rearrangements
It detects the presence of chromosomes with abnormal structure in the embryos, due to the rupture or incorrect union of various segments. There are many types of chromosomal structural rearrangements: translocations, deletions, duplications, insertions, rings or inversions, which can be balanced or unbalanced. Various chromosomal structural rearrangements result in a disease.
Recommendations:
- One of the members of the couple is a carrier of a chromosomal structural rearrangement.
Chromosomal structural rearrangements:
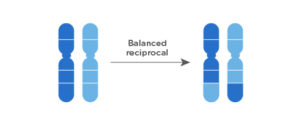
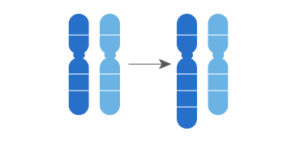
Translocations: occur when two segments of one of the chromosome pairs break off and change places. In this case, the change does not affect the genes of this chromosome and they can keep working well: it is balanced.
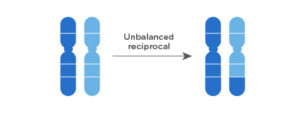
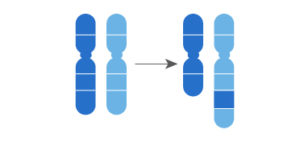
In the following example, two segments of two chromosomes break off and change places. However, there is a gain or loss, as the case may be, of the genetic material in the chromosomes: it is unbalanced.
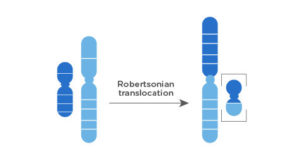
In the last example, a fusion of two acrocentric chromosomes (with one arm only) occurs at the end of the arm, which increases the risk of trisomy of the involved chromosomes.
Deletions: a chromosome segment, on breaking and trying to reconstruct itself, gets lost and so, the genes in the area are affected.
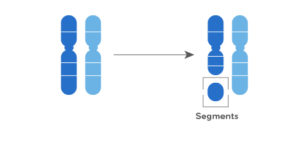
Duplications: a segment of a chromosome duplicates, resulting in extra genetic material in the area.
Insertions: a portion of the chromosome has detached from its usual location and reattached to another chromosome.
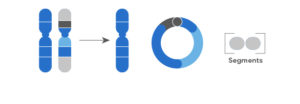
Rings: a segment of one of the chromosome pairs breaks off at the ends of both arms and tries to repair itself by rejoining the other parts, forming a circular structure. Two fragments are left out during the reparation and thus, lost. The genes found in the original chromosome cannot function properly, which leads to a disease.
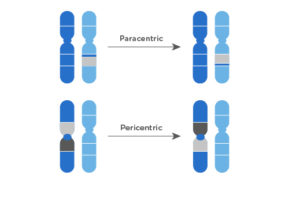
Inversions: a portion of the chromosome has broken off, turned upside down and reattached. Depending on the type, the union can result in a repaired (balanced) or unbalanced rearrangement.