
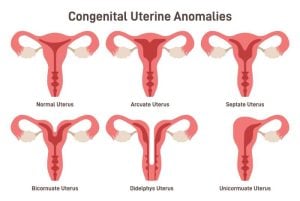
If you have a heart shaped uterus, also known as a bicornuate uterus, it means that you were born with a uterus in which the two sides did not completely fuse together as they normally do. In a heart shaped uterus, the two sides are joined at the lower end, but the top has an indentation resulting in the characteristic heart shape.
An irregularly-shaped uterus is relatively uncommon. Only around 3% of women have any sort of abnormality in the shape, size or formation of their uterus. Within this 3%, a bicornuate uterus is the most common irregularity. Normally symptom and trouble-free, for those with a heart shaped uterus, pregnancy is the time when complications can arise. For doctors to detect a heart shaped uterus, ultrasound is the most often used diagnostic tool. Without this, in the absence of pregnancy, you may not even know you have it.
Causes of a heart shaped uterus and risk factors
A heart shaped uterus is a congenital abnormality, meaning it was present before birth. It is the result of a baby girl’s uterus not developing normally in the womb. The two tubes, or ducts, called the paramesonephric ducts, that are destined to fuse together to form the womb, fail to fuse together completely. This leaves two upper parts with a horn shape diverging at either side. As it is congenital, there is nothing you or your mother could do or could have done to prevent or change this.
However, in some cases, this anomaly arises from other risk factors, such as:
- exposure to radiation during embryonic development
- intrauterine infections during pregnancy
- administration of certain medications, such as diethylstilbestrol or thalidomide
What are the symptoms of a heart shaped uterus?
This condition does not usually cause any symptoms at all, at least before pregnancy. Because of this, most women with a heart shaped uterus will not know about it unless they have an ultrasound or other imaging diagnostic test. However, some women with a bicornuate uterus do notice symptoms, including:
- Painful periods or irregular menstrual bleeding.
- Pain during sexual intercourse
- Abdominal discomfort
- Repeated miscarriage
Women with a heart shaped womb have always had it. For this reason, they may not notice anything unusual in the first three of these symptoms, which could seem normal to them.
How is a heart shaped uterus diagnosed?
Naturally, if you do have any of the symptoms which some women experience, you should consult your doctor. Your doctor could carry out a variety of tests to confirm whether you have a uterine irregularity. These include:
- An initial pelvic examination.
- A hysterosalpingogram, a specialist type of X-ray which uses dyed liquid to enable the doctor to visualise the shape of the womb and fallopian tubes.
- An ultrasound scan, in which high frequency sound waves create an image of the uterus.
Does a heart shaped uterus affect your fertility?
Most medical authorities agree that, although some other abnormalities of the womb may be associated with infertility, a bicornuate uterus does not usually have any adverse impact on your chances of conceiving in the normal way, or of the embryo implanting successfully in the lining of the uterus. Therefore, in this sense your fertility is not affected, but the risks associated with the condition come during the course of pregnancy.
Pregnancy with a heart shaped uterus
Your ability to conceive will not be affected by having a heart shaped uterus. However, it does bring some dangers to a successful pregnancy, with a raised chance of miscarriage. Researchers believe that this is because there is a reduced capacity inside the womb. Also, the unusual shape may lead to irregular uterine contractions.
Risk of miscarriage
Unfortunately, it is difficult to know the extent of the risk of miscarriage in each individual case. A study conducted by the UK’s Royal College of Obstetricians & Gynaecologists estimates the risk to be anywhere between 1.8% and 37.6%. This wide range is because the only available studies so far have included women with one, two or three miscarriages. They don’t differentiate statistically between first-trimester miscarriages and second-trimester miscarriages. The study does note, however, that second-trimester miscarriage appears to be more common in women with uterine malformation. Although, this may also be a result of the cervical weakness which is often also present.
Cervical insufficiency
The weakness of the cervix which is often seen in women with a heart shaped uterus is known as cervical insufficiency. Normally the cervix, the lower part of the uterus which opens into the vagina, is closed and firm during pregnancy. It only starts to soften and open as you prepare to give birth. If you have cervical insufficiency, it may start to open too soon, leading to a miscarriage or premature birth.
Increased likelihood of Caesarean Section
A heart shaped uterus also brings an increased chance that the baby will settle into a breech position. This means that the baby’s bottom or feet, instead of the head, are facing downwards towards the cervix before birth. In this case, doctors monitoring your pregnancy may be more likely to recommend a Caesarean Section.
How can a heart shaped uterus be treated?
As previously mentioned, a heart-shaped uterus can complicate pregnancy. Below, we explain the type of monitoring that is typically carried out when pregnancy occurs with this condition.
Surgical interventions
Surgery is not usually recommended for those with a bicornuate uterus. When surgery is used for women with a history of miscarriage, a procedure called a Strassman metroplasty can correct the condition. The success rate in terms of achieving a successful pregnancy and birth following the procedure is around 88%.
Non surgical approaches
If you are pregnant with a heart shaped uterus, your pregnancy will be classed as high risk. Your medical team will closely monitor your progress. This will probably include frequent ultrasound scans to monitor your baby’s position.
If you have a history of miscarriage or your cervix begins to open too soon, your doctor may recommend preventive treatment. This could be in the form of cervical cerclage, in which the cervix is closed with strong sutures.
Contacting IVI for fertility information
Don’t forget that the complications we have outlined here only affect a minority of women with a heart shaped uterus. The majority can expect a trouble-free pregnancy and birth. But if you have any lingering doubts about how a bicornuate womb may affect your fertility, do get in touch with us at IVI.



1 Comment
Even though your ability to conceive will not be affected by having a heart shaped uterus, it does bring some dangers to a successful pregnancy, with a raised chance of miscarriage. Santhathi is one of the best ivf center and gives a good treatmrnt on fertility