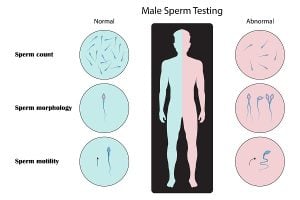
Sperm motility is the ability of sperm to move, in a straight line or a large sweeping curve. It is one of the three measures of sperm health, the other two being sperm count and sperm morphology, i.e. having a normal shape. Motility is important for fertility because if sperm have it poor, they are unable to swim through the woman’s cervix into the uterus and on into the fallopian tubes to fertilize a waiting egg.
What is a low sperm motility?
Sperm motility refers to the ability of spermatozoa to move and navigate effectively. It is assessed in terms of the speed, progression, and pattern of sperm movement. Sperm motility is considered an important factor in male fertility, as sperm must be able to move efficiently to reach and fertilize the egg.
There are two different types of sperm motility, based on the quality of movement:
- Progressive motility refers to sperm that swim mostly in a straight line or large circle
- The term non-progressive motility applies to sperm that swim in small, tight circles
For sperm to get through the cervical mucus, they need to show a minimum progressive motility of 25 micrometres per second. Low motility, known as asthenozoospermia, is diagnosed when fewer than 32% of sperm in a sample can move in this way.
How does it affect fertility?
Low sperm motility can have a significant impact on fertility. When sperm have reduced ability to move and swim, it becomes more difficult for them to reach the egg and achieve fertilization. Studies have shown that low motility is a common cause of male infertility, contributing to approximately 40% of cases worldwide. Sperm motility has been declining in recent years in Europe. A comprehensive study conducted across several European countries found that sperm motility has decreased by 0.2% per year on average over the past 15 years.
The good news is that, despite this, there are still options available for couples to increase their chances of getting pregnant. The most frequently recommended treatments would probably be intrauterine insemination (IUI), also known as artificial insemination, or in vitro fertilisation (IVF). The most recommended in your particular case would be a matter for consultation with a fertility doctor, and would depend on the personal history and circumstances of both you and your partner.
Causes of low sperm motility
Fairly frequently, low sperm motility is associated with a low sperm count. Both of them make conception more unlikely. The causes of both conditions are not easy to pinpoint and can follow from a variety of circumstances. These include injury to the reproductive organs, especially the testicles. This can come about because of:
- Diseases such as testicular cancer.
- Injury resulting from surgery to the testicles.
- Congenital disorders such as undescended testicles or hormonal imbalances
- Varicocele, a condition in which veins inside the testicles become swollen
- Infection of the testicles including epididymitis, an inflammation of the tubes carrying sperm, and some STIs such as gonorrhea and HIV.
Lifestyle factors can have a similar impact on motility, morphology, and sperm count. Smoking (including the use of marijuana) and the use of other recreational drugs, as well as overconsumption of alcohol damage significantly spermatozoa. Prolonged consumption of other drugs or toxic substances, such as anabolic steroids, can also be highly detrimental to sperm quality and specifically to motility. Occupational hazards including exposure to dangerous chemicals such as cleaning fluids and the necessity of spending long periods of time driving or sitting for other reasons.
Obesity and depression, as well as some medications, have also an adverse impact on sperm quality, including motility.
Diagnosis
The spermogram, or semen analysis, is the test performed to assess the motility of spermatozoa and, generally, to diagnose male infertility. This analysis involves evaluating a sample provided by the patient in the laboratory.
The ejaculate sample is obtained through masturbation, following a period of sexual abstinence of 3 to 5 days. In the laboratory, the shape, mobility, and number of spermatozoa are studied. These are the parameters that determine if a sample is normal:
- 39 million spermatozoa present in the ejaculate
- 32% in progressive motion
- At least 4% with normal morphology
If the figures are lower, the probability of fertilizing an egg is reduced.
How can motility be improved?
It’s clear from the summary of causes above that some instances of low sperm motility can be addressed and improved, while others are not so easy to tackle. The measures that you can take for yourself to improve sperm motility include:
- Eating a healthy diet, with an emphasis on fresh fruit and vegetables, wholegrain cereals, fish and nuts. Alongside this, avoiding highly processed foods and those containing phytoestrogens such as soy products, and foods contaminated with pesticide residue. Washing all pesticide-treated fruit and vegetables before consumption can reduce your exposure.
- Stopping smoking is one of the most important steps you can take. Smoking causes a variety of fertility problems in both men and women, including causing a reduced sperm count and reduced sperm motility. If you are aiming to improve your health before trying to conceive, it’s worth remembering that sperm take around three months to mature. For this reason, you should quit smoking at least three months before trying to conceive.
- If you’re overweight, with a BMI of 25 or more, talk to your doctor about a weight loss programme. This will help you to improve motility.
- If you can avoid overheating of the scrotum for long periods, you could improve sperm motility. The ideal temperature for sperm is just below body temperature. Therefore your testicles are outside your body, because to produce the best quality sperm they need to be kept cool. If your work requires you to operate in a hot environment, it’s important to take regular breaks outside. By the same token, if you sit still for long periods, remember to get up and move around frequently.
- Managing stress levels can potentially help improving sperm motility.
Treatment for low sperm motility
If you have a low sperm count or poor sperm motility, at IVI we offer various treatments that can help you become a father.
- Intrauterine insemination: Through this technique, selected sperm are directly deposited into the woman’s uterine cavity, allowing them to come into contact with the egg and facilitating fertilization.
- In vitro fertilization (IVF): This procedure involves fertilizing the egg with sperm in a laboratory setting, and then transferring the resulting embryo into the woman’s uterus.
- Intracytoplasmic Sperm Injection (ICSI): In this case, it is a form of IVF where the best sperm is selected and microinjected into the egg to achieve fertilization in the laboratory.
- These treatments provide options for individuals and couples facing challenges with sperm quality and motility, offering hope and the possibility of achieving parenthood.
The major difference in sperm quality between trying to conceive naturally and both fertility treatment options is that your sperm sample can be prepared in advance to increase the chances of conception. In our IVI clinics, the andrology laboratory achieves this goal. They process your sperm sample to optimize its quality and hence heighten the probability of fertilization. During the preparation, our andrologists concentrate the sperm to priorities those with the best motility and discard the less healthy ones. For some treatments, for example IVF using the ICSI technique, the individual healthiest sperm can be selected for microinjection into each egg individually to facilitate conception.
If you have been diagnosed with low sperm motility or have any other concerns about male fertility, don’t hesitate to get in touch with us at IVI. Nine out of ten couples who contact us with fertility problems fulfill their quest to become parents. The chances that we can help you are very good!


Comments are closed here.